Cardiovascular diseases (CVDs) are the leading cause of death in the U.S. and around the world. According to the World Health Organization, an estimated 17.9 million people die from CVDs each year. The vast majority of these deaths are due to heart attacks and strokes.

Heart attacks and strokes happen when a buildup of plaque, or fatty deposits, on the inner walls of arteries prevents blood from flowing to the heart or brain. To remove these blockages, surgeons need a real-time, high-resolution view into the artery. But conventional optical elements currently used in endoscopes are too bulky and stiff to reach diseased arteries deep in the heart or brain.
Recently, an interdisciplinary research team at the University of Washington (UW), led by Arka Majumdar, an associate professor of electrical and computer engineering and physics, was awarded $3.6 million in funding from the National Science Foundation (NSF) to take on this challenge. Using the emerging nanophotonics and metamaterial technology meta-optics in combination with advanced computational post-processing, the team aims to develop a dramatically smaller endoscope to image previously inaccessible areas of the heart and brain.
Unlike the thick glass lenses of traditional cameras, meta-optics are nearly two-dimensional, studded with over a million tiny cylindrical structures that capture and re-emit light at the nanometer scale. The unique geometry and arrangement of these nanostructures determines how these extremely thin optical elements, less than one millimeter thick, interact with light to produce an image.
“Others have attempted to incorporate meta-optics in endoscopes, but never before has machine learning been used to both design the meta-optics and improve image quality on the backend,” said Majumdar. “On their own, meta-optics suffer from poor resolution and color aberrations. But by merging meta-optics with machine learning, we will make a miniaturized imaging system that can produce high-resolution, full-color images with an extended field of view.”

To build a miniaturized scope that can be used by surgeons, Majumdar is bringing together a highly diverse team that includes academic researchers, medical professionals and startups all based in Washington State. Majumdar’s co-investigators include nanofabrication expert Karl Böhringer, a professor of electrical & computer engineering and bioengineering at the UW, and Eric Seibel, a professor of mechanical engineering at the UW and expert in ultrathin and flexible medical imaging devices. Machine learning expert Steve Brunton, also a professor of mechanical engineering at the UW, will play a key role in optimizing the meta-optics design. The research team will work with neurovascular and cardiovascular surgeons Drs. Luis Savastano and John Petersen to better understand the needs of their end user. They will also collaborate with UW spinouts Tunoptix, cofounded by Majumdar and Böhringer, and VerAvanti, which is commercializing a technology pioneered by Seibel known as Scanning Fiber Endoscopy (SFE), to figure out how to manufacture and commercialize these scopes at scale.
“Current scopes utilize 50-year-old technology consisting of bundles of glass optical fibers that form a rigid tip, limiting where the scopes can go,” said Seibel. “SFE uses lasers and a micro-electro-mechanical scanner to reduce the length of this rigid tip from nine to about five millimeters. Meta-optics will reduce this even further to two and a half millimeters or less, giving surgeons full access to areas of the body that currently cannot be visualized at all.”
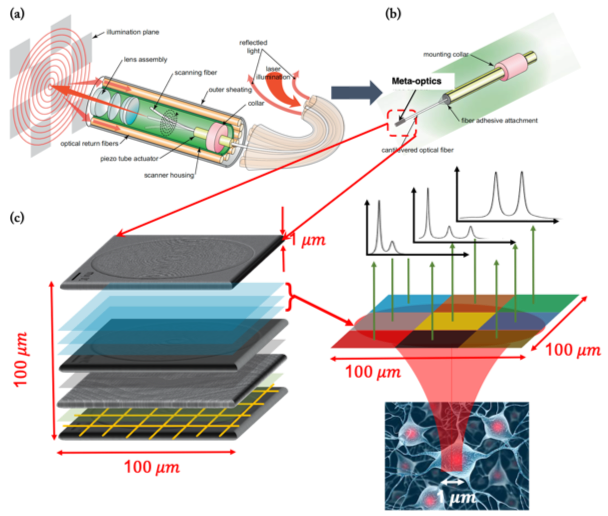
Key to the viability of this device in the real world is that it is both inexpensive to produce and disposable. Meta-optics are fabricated using the same semiconductor manufacturing techniques that produce computer chips.
“We are fortunate to have access to the largest publicly accessible nanofabrication facility in the Pacific Northwest right here on the UW campus,” said Böhringer, who as the director for the Institute for Nano-engineered Systems oversees the Washington Nanofabrication Facility (WNF), an open-access user facility that provides academic researchers and industry professionals access to nanofabrication tools and expertise. “Microfabrication has successfully been used to mass produce semiconductors, drastically reducing their cost. Certainly, there is a lot of evidence that meta-optics can similarly be made at scale, but it remains an open question exactly how to do this.”
The team will begin by working to demonstrate that meta-optics can be used to reduce the tip length of both conventional endoscopes and scanning fiber endoscopes. They also hope to establish the feasibility of their longer-term goal of integrating computational processing and meta-optics to achieve the smallest and most agile endoscope possible. The team’s clinical and industry collaborators will provide input to help ensure a useful and feasible end product. Eventually, clinicians working at the frontiers of endovascular surgery will help test the device.
“There are lots of potential applications for meta-optics – everything from cell phone cameras to satellites – but I think that its integration in biomedical devices such as endoscopes is where meta-optics will have the biggest impact,” said Majumdar. “The need is clear. Miniaturization of the optical elements in endoscopes could transform the treatment of cardiovascular disease and ultimately save lives.”